A Situation Update On Covid-19 Variants And Vaccines
(Posted on Wednesday, July 28, 2021)
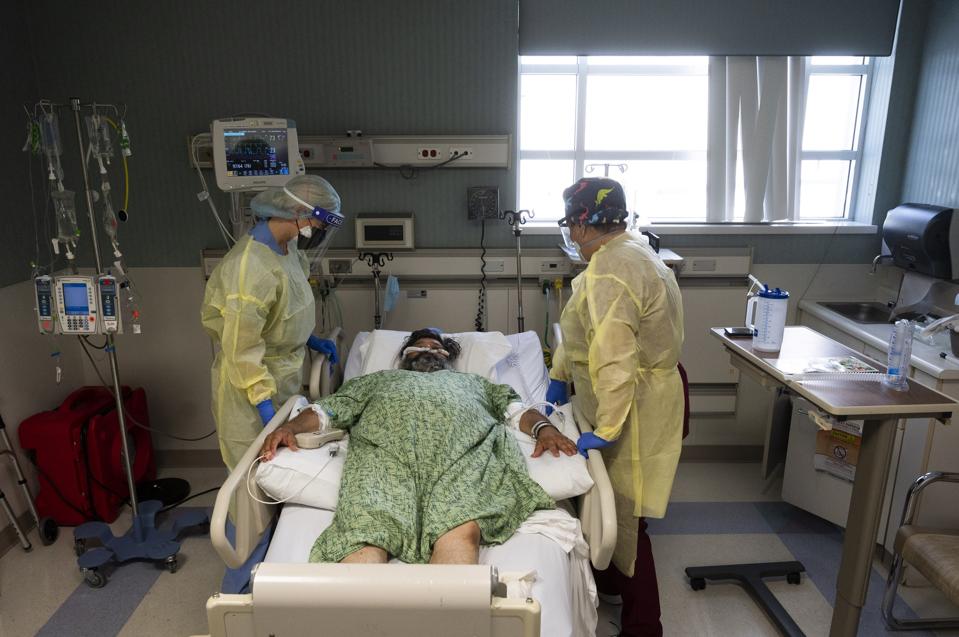
Orange, CA – July 21: Jamie McDonough, RN, left, and Nurses Assistant Vanessa Gutierrez, check on a COVID-19 patient in the COVID ICU at St. Joseph Hospital in Orange, CA on Wednesday, July 21, 2021. COVID-19 cases have risen in recent weeks due, in
MEDIANEWS GROUP VIA GETTY IMAGES
The article that follows is complex, so I will first and foremost summarize its major points. The fundamental advice I must begin with is that if you’re not vaccinated, get vaccinated, because it will likely prevent your hospitalization or death.
Second, that being said, some vaccines are much better than others. The mRNA vaccines have proved to be much better than the rest, including the adenovirus and inactivated whole virus vaccines.
Third, all currently approved vaccines wane in efficacy over time, for some populations more than others. Those who are 65 and older, along with others high-risk groups, can anticipate having a level of immune protection that is less robust and sooner to fade. Boosters will very likely be required, first for older adults, then the general population, within six months of their last shot.
Lastly, it is very likely that new and even more dangerous viruses than the Delta will emerge, and it’s unclear how well existing vaccines will protect from hospitalization and death from such new variants. All these considerations and more I will elaborate on in the succeeding paragraphs.
As we close in on the end of another month with Covid-19, the outlook for the rest of the year is decidedly unclear. Though about a quarter of the world’s population has received at least one dose of a Covid-19 vaccine, in many countries the virus is still circulating at worrisome, if not outright alarming, speeds. Even in countries with high vaccination rates, like the United Kingdom and Israel, new variants of SARS-CoV-2—each, it seems, more infectious than the next—have contributed to sharp increases in new cases, some of which are breakthrough infections.
How to explain this paradoxical state of affairs? It depends where you turn for answers. Public Health England published a study in June declaring that two doses of either the Pfizer or AstraZeneca vaccine were more than 90 percent effective at preventing severe disease and hospitalizations from the Delta variant. But last month, the number of daily new Covid-19 cases in the UK still reached a peak that rivaled the country’s record highs last winter. Even though new infections now appear to be on the decline, in the past week hospitalizations rose more than 30 percent, sending National Health Services executives and health workers into yet another downward spiral.
Recent data reported by Israel’s Ministry of Health on July 23 tells a slightly different story about vaccine efficacy against the Delta variant. According to their study, which has yet to be released in full, the Pfizer vaccine is 88 percent effective at preventing hospitalizations and 91 percent effective at preventing critical illness from the Delta variant, but just 39 percent effective against infection—a significant drop from previous estimates of 64 percent effectiveness. The report came as hospital admissions rose more than 50 percent across the country in the span of one week.
It is in light of Covid-19 surges not just in Israel and the UK, but across the globe that the topic of immune protection has resurfaced, with new and increasing urgency, in discussions of pandemic control. Research on the mRNA vaccines created by Pfizer and Moderna has repeatedly confirmed that they trigger the most robust immune response against SARS-CoV-2. But how long vaccine-mediated immune protection lasts remains uncertain, especially for their less effectual counterparts: AstraZeneca and Johnson & Johnson’s adenovirus vaccines, China’s Sinopharm vaccine, India’s Covaxin vaccine, and so on.

Comparison of reductions in efficacy over time based on data from the modeling study
“NEUTRALIZING ANTIBODY LEVELS ARE HIGHLY PREDICTIVE OF IMMUNE PROTECTION FROM SYMPTOMATIC SARS-COV-2 INFECTION” HTTPS://WWW.NATURE.COM/ARTICLES/S41591-021-01377-8
Not all vaccines, it has become clear, are created equal. In May 2021, a study published in Nature Medicine made this claim based on the aggregated clinical trial results of seven different Covid-19 vaccines. Using predictive modeling techniques to plot the strength and duration of their immune protection over a theoretical timeline of 250 days, the study’s authors showed that some vaccines dropped to 50 percent efficacy much earlier than others. Leading the pack were Pfizer and Moderna’s mRNA vaccines, which performed at 95 percent efficacy initially and took a full 250 days to fall to 50 percent. The AstraZeneca vaccine rounded out the bottom with 62 percent initial efficacy and a half life of 48 days, though the Sinopharm vaccine fared even worse, having just 50 percent efficacy to begin with.

Relationship between neutralization level and protection from SARS-CoV-2 infection
“NEUTRALIZING ANTIBODY LEVELS ARE HIGHLY PREDICTIVE OF IMMUNE PROTECTION FROM SYMPTOMATIC SARS-COV-2 INFECTION” HTTPS://WWW.NATURE.COM/ARTICLES/S41591-021-01377-8
The authors of the Nature Medicine study, like many researchers before them, use antibody titers as their selected measurement of immune protection, rather than T cell or memory B cell counts. While all of the above ultimately make inexact correlates of protection, based on vaccine data and previous encounters with viruses like influenza, antibodies are most likely the best we’ve got. And until a standardized immunological assay is created for SARS-CoV-2, they’re the best we’re going to get.
Early studies of Covid-19 patients established that antibody levels generated by natural infection are quick to fade. Today, studies of vaccinated individuals are beginning to emerge that report similar findings. According to one conducted across the UK in June and published in the Lancet on July 15, antibody levels of adults fully immunized with either the Pfizer (BNT162b2) or AstraZeneca (ChAdOx1 nCoV-19) vaccines dropped significantly over the course of 70 days. For participants who received two doses of Pfizer, the drop was two-fold; for those who received AstraZeneca, five-fold.

Total antibody counts following second doses of BNT162b2 (Pfizer) and ChAdOx1 nCoV-19 (AstraZeneca) vaccines
“SPIKE-ANTIBODY WANING AFTER SECOND DOSE OF BNT162B2 OR CHADOX1” HTTPS://WWW.THELANCET.COM/JOURNALS/LANCET/ARTICLE/PIIS0140-6736(21)01642-1/FULLTEXT#CORONAVIRUS-LINKBACK-HEADER
But just as the strength and duration of immune protection varies from vaccine to vaccine, the Lancet study suggests it varies from individual to individual, too. The supplementary figures below show that antibody levels are generally lower and faster to wane in adults 65 and older. Strikingly, by the end of the 70-day period, the lower limit of antibody levels in older adults who received the AstraZeneca vaccine reached nearly zero. The same was true for individuals categorized as “clinically extremely vulnerable” due to presenting certain comorbidities, like chronic respiratory disease, obesity, diabetes, and specific cancers. In other words, the populations at highest risk of developing severe illness upon infection were ostensibly the least protected.

Total antibody counts following second doses of BNT162b2 (Pfizer) and ChAdOx1 nCoV-19 (AstraZeneca) vaccines, stratified by age (left) and vulnerability (right)
“SPIKE-ANTIBODY WANING AFTER SECOND DOSE OF BNT162B2 OR CHADOX1” HTTPS://WWW.THELANCET.COM/JOURNALS/LANCET/ARTICLE/PIIS0140-6736(21)01642-1/FULLTEXT#CORONAVIRUS-LINKBACK-HEADER
This is to say nothing of the variants. In a virtual presentation for the Zuckerman Institute at Columbia University, infection analytics expert Miles P. Davenport made one more addition to the predictive model I discussed previously—the CUREVAC vaccine. Like the Pfizer and Moderna vaccines, CUREVAC was designed using mRNA, raising expectations of its success. But in phase 3 clinical trials, it demonstrated only 47 percent efficacy. One interpretation of the lackluster performance is that previously approved vaccine candidates did not have to contend with variants in their respective clinical studies. What will happen if more variants emerge that are even more infectious than what we’re seeing now?

Performance of CUREVAC vaccine
“RELATING IN VITRO NEUTRALISATION LEVEL AND PROTECTION IN THE CVNCOV (CUREVAC) TRIAL” HTTPS://WWW.MEDRXIV.ORG/CONTENT/10.1101/2021.06.29.21259504V1
I cannot stress enough that any Covid-19 vaccine—meaning those deemed safe and effective, of course—is better than no vaccine. And rates of hospitalization and incidence of severe illness are indeed both down from their respective highs last year. But the combination of a fast-evolving virus and, if the antibody counts are to be believed, fast-fading immunity is too inauspicious for my liking.
Though the global vaccine rollout remains uneven and inequitable, booster shots—especially for the elderly and other high-risk populations—are inevitable. When booster shots are eventually made available, anyone over the age of 65 or at a similar risk level should seek them out. The rest of us should monitor our antibody counts and take action when we register a significant drop. After all, it is always better to be safe than sorry.
Originally published on Forbes (July 28, 2021)