Autoantibodies May Be The Driver Behind Severe Covid-19 Reactions
(Posted on Tuesday, January 26, 2021)
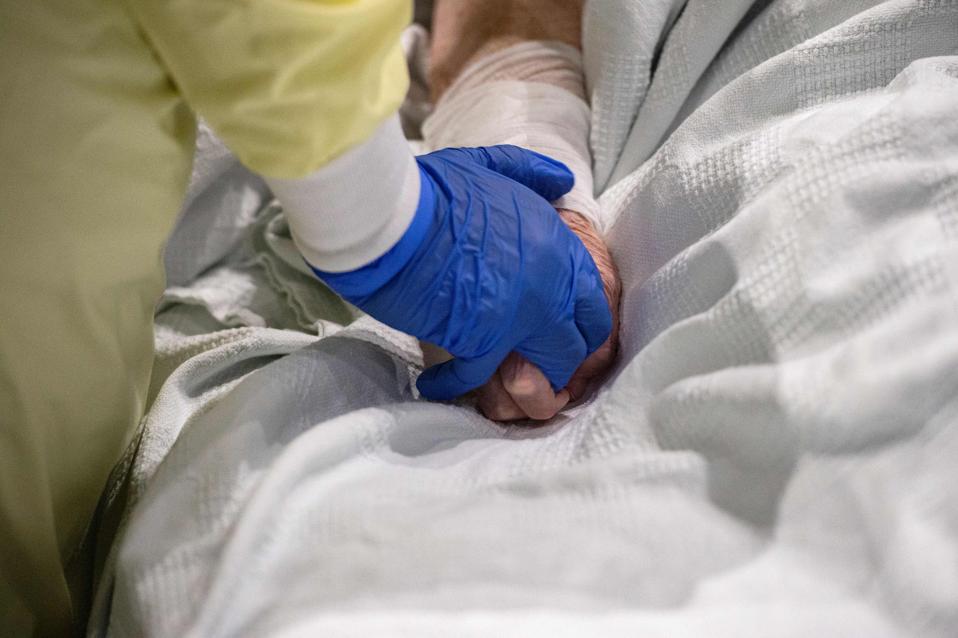
Medical workers care and comfort a patient who is suffering from the Covid-19 virus at the UMASS Memorial DCU Center Field Hospital in Worcester, Massachusetts on January 13, 2021. – The field hospital currently has fifty non critical patients
AFP VIA GETTY IMAGES
While vaccine distribution and President Biden’s inauguration occupied most of the media’s attention, January marked the peaks of hospitalization and deaths among Covid-19 patients in the United States. Over 130,000 were in the hospital with severe Covid-19 symptoms in the past two weeks. Emerging evidence suggests one cause of severe Covid-19 reaction may be autoantibodies or antibodies that attack the body and not an invading pathogen. What do we know about autoantibodies, and how can our understanding of them inform Covid-19 research moving forward?
A recent study out of NYU analyzed the sera of 86 hospitalized Covid-19 patients. Researchers were on the hunt for autoantibodies, self-attacking proteins mistakenly turn on the body in their attempt to root out pathogens. It is unknown how many people have these antibodies present in their immune systems, though ongoing research is looking into the matter. The NYU researchers hoped their presence could provide some clarity on why some patients get so sick from SARS-CoV-2 infection.
They indeed found autoantibodies geared against the annexin A2 protein, which stabilizes cell membranes and blood vessels in the lungs. On average, hospitalized Covid-19 patients had a significantly higher level of these autoantibodies than non-severe patients, and their targetting of the lungs may be one of the causes for Covid-19 related respiratory issues.
Autoantibodies targeting interferon responses are noted by several studies as a significant factor in severe Covid-19. The interferons are warning signals that alert the immune system whenever a pathogen invades, which I’ve written about here. A study out of Science showed autoantibodies reducing interferon circulation in the blood to extremely low levels, meaning the pathogen could easily spread throughout the body without having to worry about the substantial immune response. Autoantibodies also seem more prevalent in older adults, which falls in line with who is more likely to have a severe Covid-19 reaction.
A major question remains unresolved. Are annexin A2 and interferon autoantibodies activated by Covid-19 infection, pre-existing in the patient, and therefore predisposing them to infection? Or are they actually induced by the infection itself? That is an interesting question for these specific autoantibodies, but also for autoantibodies in general found in patients ill with Covid-19. To this point, the existence of autoantibodies in patients prior to arriving at the hospital is unreported.
Why do autoantibodies arise? Some are created when the immune system recognizes similar structures in the invading pathogens and human proteins. Some antibodies may be produced by a flood of cellular debris released upon pathogen destruction of cells. In the case of Covid-19, we don’t know the answer.
A leading theory for autoantibody development in reference to Covid-19 relates to disfunction in the follicular node when a patient becomes infected. The follicular node is the B cell’s learning center; it is where an antibody learns to neutralize a pathogen. In hospitalized patients, this node is often damaged. This may lead to a B cell less equipped to create virus-fighting antibodies properly and may produce harmful autoantibodies that prompt severe symptoms.
While research doesn’t seem to lean one way or the other on why we have autoantibodies waiting to pounce, studies are in the midst of production to find the answers. Rockefeller University in New York was one of the first to observe autoantibodies in Covid-19 patients back in September and are currently screening as many as 40,000 patients to see how many had preexisting autoantibodies.
If autoantibodies are found to be a significant driver of severe Covid-19 symptoms, pharmaceutical developers should be inclined to research further Covid-19 therapies geared towards them. Treatments that boost specific proteins in weakened immune systems may just be creating more targets for autoantibodies to attack. Testing for these autoantibodies could even be a strong indicator to identify at-risk people for severe Covid-19.
Furthering our understanding of how Covid-19 works and why some experience severe Covid-19 symptoms may lead to more effective treatments for patients. Even if an autoantibody therapy or test could save a few lives, the research is worth doing. Ultimately, autoantibody research may open doors for future understanding of this virus and how it affects us.
Originally published on January 26, 2021.

