The Role of AI in Improving Diabetic Retinopathy Screening Programs
(Posted on Saturday, November 25, 2023)

Image of human eye in process of scanning. Mixed media
This article was published on Forbes on 11/20/2023.
This story is part of a series on the current progression in Regenerative Medicine. This piece is part of a series dedicated to the eye and improvements in restoring vision. This piece also marks part two in a small series on diabetic retinopathy.
In 1999, I defined regenerative medicine as the collection of interventions that restore to normal function tissues and organs that have been damaged by disease, injured by trauma, or worn by time. I include a full spectrum of chemical, gene, and protein-based medicines, cell-based therapies, and biomechanical interventions that achieve that goal.
Diabetes can cause diabetic retinopathy, a complication that has the potential to lead to blindness. However, early screening and proper management can prevent or slow its progression, underscoring the importance of screening programs. Screening programs play a critical role in preventing complications of diabetic retinopathy, and the efficacy of these programs can be enhanced through artificial intelligence (AI).
How Artificial Intelligence is Used in Screening Programs
In recent years, AI has emerged as a tool in the early detection and treatment of diabetic retinopathy. AI-powered computer-aided diagnosis systems are being developed to analyze retina images and identify abnormalities indicative of diabetic retinopathy. These systems use machine learning algorithms to recognize and classify features such as microaneurysms, hemorrhages, and exudates. By analyzing these features, AI can evaluate the severity of the condition and recommend appropriate treatment.
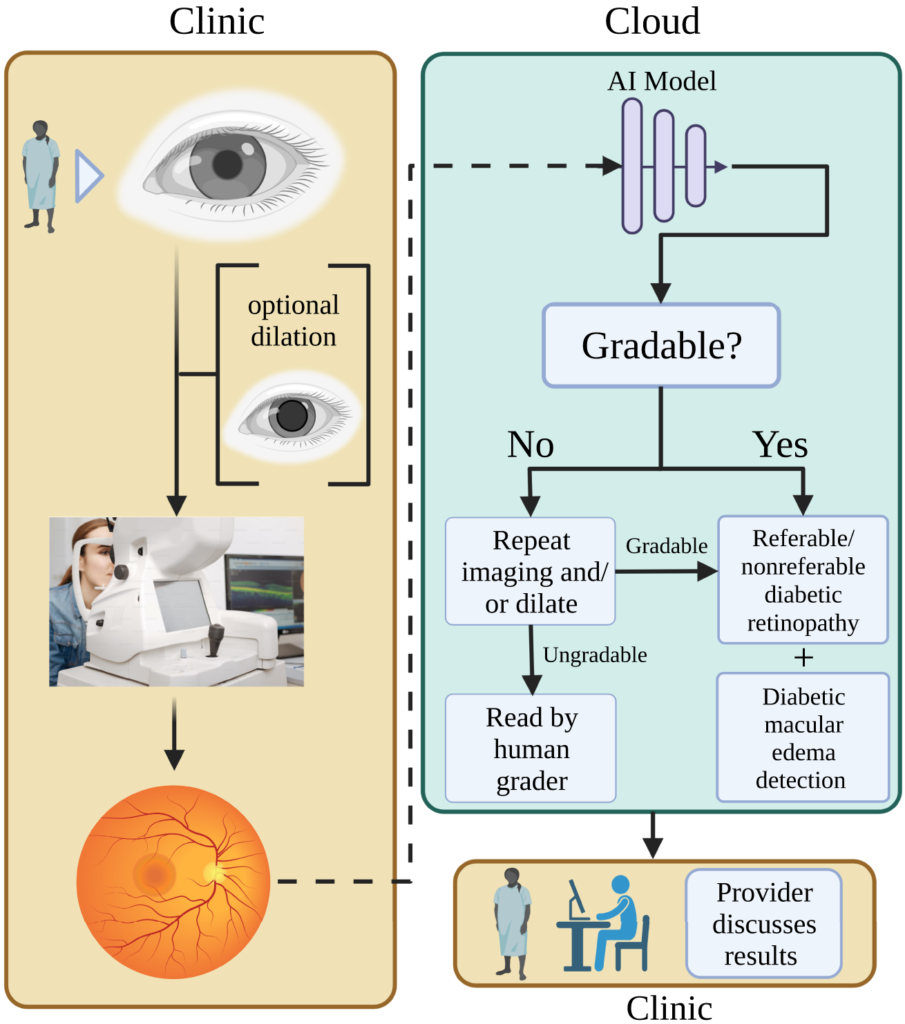
Retina images are captured and uploaded to a cloud server during a typical eye exam. These images are later analyzed by artificial intelligence using advanced machine learning algorithms, which generate comprehensive reports for clinicians. These reports highlight any potential abnormalities, which can be further evaluated by either AI or humans to determine the risk of disease or disease progression.
For patients at an elevated risk of developing the condition, it becomes possible to implement early interventions to prevent potential vision loss. This proactive approach can significantly contribute to preserving and safeguarding one’s eyesight.
Efficacy of AI-Human Partnerships in Diagnosing Diabetic Retinopathy
A recent study published in JAMA Network Open evaluated an AI algorithm’s ability to analyze non-invasive retinal imaging. The algorithm achieved an impressive sensitivity of 87.2% and a specificity of 90.7% in predicting the future development of diabetic retinopathy compared to a highly rigorous reference standard set by expert human graders.
Furthermore, a review by a team from the University of Washington in Seattle assessed the performance of various AI algorithms designed explicitly for diabetic retinopathy. The AI output was evaluated against the reference standard established by ophthalmologists. The findings revealed that the algorithms consistently outperformed the specialists in multiple studies. However, the review does express apprehension regarding the limitations and accessibility of these technologies in clinical practice.
By merging the power of AI technology with the expertise of healthcare professionals, more accurate diagnoses and effective treatment plans can be developed. Artificial intelligence can assist in the early identification of medical conditions like diabetic retinopathy. This can result in timely interventions and ultimately improve patient outcomes.
Early Detection in Critical
Early detection of diabetic retinopathy is vital for successful treatment and improved patient outcomes. Not only does it reduce the need for frequent checkups, but it also aids in lowering healthcare costs. Early detection can also reduce the risk of vision loss for diabetics by 95%
Healthcare providers can use predictive AI models and diagnostic assistance to accurately identify patients who require monitoring and direct them to appropriate care. A team from New York conducted a study that showed how diabetic retinopathy risk can be determined by fundus photography. By training AI on a machine learning algorithm, the images can be assessed for risk.
AI systems can help reduce the workload of healthcare professionals, enabling them to spend more time on quality patient care, which is critical given the growing shortage of medical personnel. At the same time, the AI takes on the laborious task of analyzing medical images. This approach optimizes healthcare resources by prioritizing patients needing immediate attention while avoiding unnecessary checkups that can drain time and finances. Additionally, leveraging predictive AI models aids in identifying potential health risks early on, resulting in further enhancements to patient outcomes.
Limitations of Artificial Intelligence in Diagnosing Diabetic Retinopathy
The use of AI in managing diabetic retinopathy has been a topic of debate due to its controversial effectiveness. While AI can screen patients for diabetic retinopathy, researchers have reported that relying solely on AI may lead to overdiagnosis and overtreatment of patients. This is because AI algorithms may classify lesions as clinically significant when they are not.
Another limitation of AI in diabetic retinopathy management is its ability to analyze retina images and make thorough treatment recommendations. While AI can detect certain features of the retina, it cannot evaluate the patient’s medical history, current symptoms, or other factors that may be critical in making treatment decisions.
Therefore, healthcare professionals should view AI as a supplementary tool to provide personalized care to patients with diabetic retinopathy and not as a replacement for human clinicians.
Tomorrow Brings Better Diagnostic Tools
By leveraging AI’s capacity to identify high-risk groups and facilitate early diagnosis and monitoring, we can reduce the prevalence of vision loss and blindness among diabetic individuals. But it doesn’t stop there.
These systems can also enhance screening accuracy, efficiency, and affordability, making them accessible to a broader population. However, for optimal patient and societal benefits, it is imperative that AI technology adheres to sound ethical guidelines and integrates effectively into healthcare settings.
Our aim should be to refine the AI system’s diagnostic accuracy further and combine it with interventions promoting healthy lifestyles, thus preventing diabetic retinopathy’s development and progression.
To learn more about the eye, read more stories at www.williamhaseltine.com

