Who Are The Vaccinated That Still Become Infected?
(Posted on Saturday, January 9, 2021)
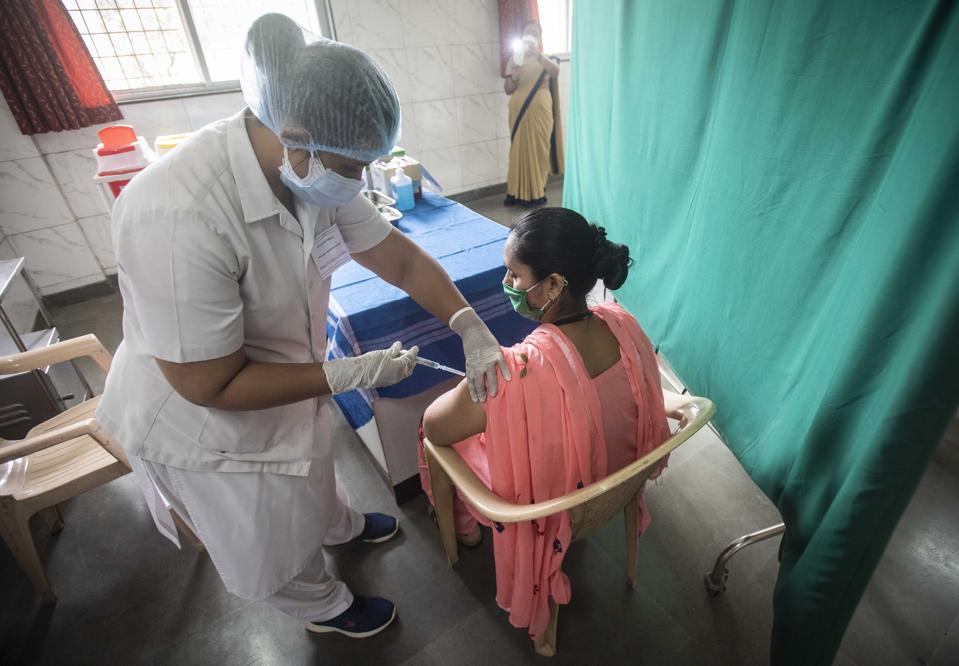
PUNE, INDIA – JANUARY 8: Healthe workers during dry run of Covid-19 vaccination at Yerawada, on January 8, 2021 in Pune, India. (Photo by Pratham Gokhale/Hindustan Times via Getty Images)
HINDUSTAN TIMES VIA GETTY IMAGES
Vaccine development was one of the few shining lights during a dark past ten months. After a remarkably rapid design and trial period, pharmaceutical companies Moderna and Pfizer announced efficacy percentages in the high 90s. A tremendous achievement, but even an efficacy of 95% means five percent of vaccinated people are susceptible to Covid-19. Some vaccines, like the Oxford-Astrazeneca and Chinese vaccines, have efficacy around 90 or even 80%.
Assuming efficacy numbers hold true, many millions will still get infected after receiving a vaccine. Five percent of a global population approaching eight billion is upwards of 350 to 400 million people. Ten to twenty percent could be as many as 800 million to 1.6 billion people. For those people who were vaccinated that were later infected, what happened?
Little data is available on those that are vaccinated, then infected. Most vaccine attention focuses on widespread distribution or lack thereof. As distribution settles down and the vaccine is available to more people, attention will likely shift to the vaccines’ success over time. Understanding those biological failures will enable scientists to improve vaccines prevent further viral spread.
Once inside the body, many factors could increase or decrease the chance the vaccine will protect. As these vaccines require two doses three weeks apart, it’s possible that patients contracted Covid-19 after their first dose when efficacy is much lower. Some experts suggest that those that have recently received a blood transfusion have impaired vaccine immune response. Some people’s immune systems may reject the vaccine antibodies altogether. There is still little known because we don’t have long term vaccination data yet.
Everyone responds differently to the virus. No two Covid-19 patients have the exact same immune response to their infection. The same could be said for vaccines. Many of the vaccines in distribution have neutralizing antibodies which help the body fend off the virus. In many cases—5 to 20% based on which vaccine is used—these antibodies may be rejected by the body’s natural immune response. This is data researchers need to be on the lookout for. If vaccines don’t cover everyone, we need to know why and how we can fix it.
There should be some national vaccine data collection system in place to help researchers learn more. Such a system could be associated with social security numbers, simply indicating which people were vaccinated, which have yet to be, and who got sick after receiving their shots. This would allow researchers to investigate the cases where vaccines didn’t help, identify factors in the pre-inoculation process that may have gone wrong with that shot, or see if the patient had some reaction to the vaccine leading to it being ineffective.
This system would also help state and federal health entities track vaccine distribution progress as they attempt to inoculate over 300 million people in the United States and nearly 8 billion worldwide. Vaccine distribution to this point has been an unmitigated disaster, with vaccination counts well below the estimations set in previous weeks. We need a change in administrative processes to catch those who fall through the vaccine safety-net.
Additionally, the emerging Covid-19 variants render understanding vaccine efficacy all the more crucial. The mutations in the structure of the United Kingdom and South African variants created a more contagious virus. It’s possible that mutations could occur to make these variants or undiscovered variants resistant to current vaccines. Pfizer released a statement attempting to dissuade concern about variants being vaccine-resistant, but their studies did not test a full array of mutations to the virus, only one individual mutation. Their findings have also yet to be peer-reviewed. The reality is, we don’t know the dangers that lie in the viral variants.
We need to learn more. If Moderna and Pfizer have access to information about those that may be less protected by their vaccines, that information needs to be released, studied, and tested. As millions are infected weekly, and thousands die every day, we need to protect those that vaccines cannot. Vaccines represent hope for many wanting an end to this pandemic. If they don’t end up working to the degree we hoped, there will be a widespread disappointment to pair with further Covid-19 devastation.
Read the full article on Forbes.
Originally published on January 9, 2021.

